Movement Is An Essential Nutrient
Posted on 21/11/2022
21 Enterprise House, Kingsway North, Team Valley, Gateshead, NE11 0SR
Vitamin D deficiency is very common in the U.K. – it’s thought that as many as 90% of our population may be deficient in vitamin D during the winter months, with this deficiency persisting in about 60% of us even during the height of summer.[1]
This deficiency is causing concern because vitamin D:
Vitamin D deficiency is a recognised cause of rickets, osteoporosis and other bone weakening conditions but there is significant research linking it to many other forms of illness as well, including:
Vitamin D acts like a hormone and cytokine (chemical messenger), and plays a pivotal role in regulating the body’s immune and inflammatory responses, cell division, nervous system activity and bone maintenance.
Almost every cell in the body appears to have vitamin D receptors, and this is why vitamin D deficiency has the potential to disrupt the function of the body in so many varying ways.
Our body makes vitamin D when our skin is exposed to the UVB radiation found in sunlight, but for this to happen our body must be getting enough direct exposure to sunlight to stimulate this process. In addition, our liver and kidneys must also be in good shape to drive the biochemistry of vitamin D synthesis within our body.
Unfortunately, our modern lifestyles often mean that these basic requirements for vitamin D production are not being met. For example:
Without a blood test you probably can’t, as you can be quite deficient in vitamin D and yet feel normal and healthy for quite some time before signs or symptoms begin to appear.
With time, you might start to feel a bit tired or “low”, or begin to notice general “muscular” aches and pains, but these symptoms are quite non specific, and can be associated with many other potential problems as well.
With further progression the physical signs of rickets or other bone weakening conditions may emerge, but this only tends to happen much later in the clinical picture after the vitamin D deficiency has been well established for some time.
In some ways it may be safest for those of us living in the U.K. to simply assume that we are deficient until proven otherwise. A simple blood test can answer the question one way or another, and once you know your status it’s fairly easy to manage your situation through lifestyle measures or vitamin D supplementation if required.
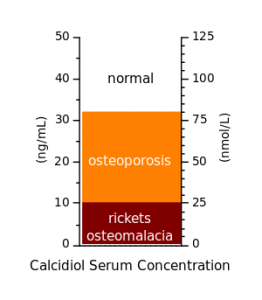
This is a difficult question to answer because no one really knows for sure, and there is discrepancy of opinion in different parts of the world.
Current UK guidelines define deficiency as having blood vitamin D levels below 25 nmol/L[3], but there are those who argue that this figure is quite conservative and that levels associated with optimal health may be more in the region of 75-150 nmol/L[4].
In many ways, any advice on this issue needs to be tailored to your individual situation, so we recommend you chat to your G.P. or other suitably qualified heath professional for information about your specific situation.

The best way to increase your vitamin D levels is to aim to get about 15-20 minutes of sunlight on your face, arms and trunk three to five times a week during those times of the year when our sun is sufficiently strong enough to stimulate Vitamin D production in the body. In northern England, that generally means between May and August.
Some foods also contain small amounts of vitamin D (eg cod liver oil, egg yolks) or are fortified with it (some margarines and cereal products), but the amount of vitamin D in these products is not that high and they do not really have much impact in raising blood vitamin D levels.
Lastly, if vitamin D levels are low vitamin D then supplementation may also be needed, especially during those months of the year when our body cannot make vitamin D naturally.

Vitamin D supplementation can be very helpful, but specific recommendations are best made once a blood test has been taken to ascertain your current blood levels of vitamin D so that any advice on the use of supplements can take this and other aspects of your general health into account.
Thankfully, both the blood test and vitamin D supplementation are relatively inexpensive processes, and knowing your blood vitamin D levels will also help you monitor the effectiveness of any recommendations that are made for you.
Yes, excessive vitamin D intake can alter the healthy ratios of calcium and phosphorous in your body and cause health problems, but this is quite rare.
It’s generally thought that a normal adult would need to be taking a lot of vitamin D (as much as 40,000 i.u per day over an extended number of months) in order to run into problems of vitamin D toxicity[5].
Therefore, a healthy adult taking 1000 to 2000 i.u. of vitamin D a day to support general health and wellbeing has a high margin of safety, with much higher levels of vitamin D than this being used under medical supervision to correct clinical deficiency.
However, given that we are all unique individuals anyone considering taking vitamin D supplements should chat to their G.P. or suitably qualified health professional first, and should consider the merits of monitoring their blood vitamin D levels periodically to ensure that they are using vitamin D supplements in a safe and effective way.
Yes – in fact it is particularly important that pregnant women and children get enough vitamin D to support healthy growth and development.
For the child, this is especially important during the “in utero” growth of the developing baby and in the early childhood and adolescent years.
For the mum, this is very important before and during the pregnancy to help her meet the demands of “building a baby inside her”. However, it is also important in the period after she has given birth, as her own physical wellbeing needs to be returned to optimal levels to in order for her to sustain optimal health in the future (and to support any subsequent pregnancies if she chooses to have more than one child!).
This aspect of the vitamin D story – coupled with the fact that there have been cases of rickets diagnosed in parts of the U.K. in recent times – is a major reason why G.P.’s and other health professionals are being encouraged to be particularly diligent in ensuring that mums to be and their children understand the importance of vitamin D and have easy access to it.[6]
If you want to take steps to improve your vitamin D levels there are a number of things you can do:
1. Do a lifestyle check.
2. Get your vitamin D levels checked.
3. Stay informed
All of these references will provide you with more information about vitamin D, but if you have further questions or wish to speak to one of our practitioners about the information contained in this article please call on (0191) 491 5111.

You’d think the Aussies – living down there in all that sunshine – would have no problem with their vitamin D levels.
Think again! As this article suggests, modern lifestyles are undermining the vitamin D status of people living in many different countries, including sunny Australia.
Nonetheless…sunny Bondi still has a certain allure!
[1] Hypponen E, Power C. Hypovitaminosis D in British adults at age 45y: nationwide cohort study of dietary and lifestyle predictors. Am J Clin Nutr. 2007 Mar;85(3):860-8
[2] The Vitamin D Council, http://www.vitamindcouncil.org/health-conditions/
[3] City Assays, http://www.vitamindtest.org.uk/q&a.html
[4] Nutri Clinical Guide – Vitamin D http://www.nutri-online1.co.uk
[5]Vieth R Vitamin D supplementation, 25-hydroxyvitamin D concentrations, and safety. Am J Clin Nutr 1999 May 69;(5):842-856 http://ajcn.nutrition.org/content/69/5/842.abstract
[6] Vitamin D – advice on supplements for at risk groups – letter from UK Chief Medical Offices February 2012 https://www.gov.uk/government/publications/vitamin-d-advice-on-supplements-for-at-risk-groups
[7] http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0152441